Compiled by Shaheen Hossain, PhD
Background
Fetal death is a major public health problem. It accounts for more than half of all perinatal deaths. The World Health Organization defines fetal death as “death prior to the complete expulsion or extraction from its mother of a product of human conception, irrespective of the duration of pregnancy.” Although this definition of fetal death is the most frequently used, it is by no means the only definition. The Centers for Disease Control and Prevention recommend reporting fetal deaths occurring at 20 weeks of gestation or greater. This policy is only a guideline and reporting practices vary among states.
Risk Factors
Several studies have established an association between fetal death and maternal age. (1,2) Other studies have shown that the risk factors for the occurrence of fetal death include previous stillbirth, congenital malformations, multiple gestations, grand multiparity (>5 prior births), no prenatal care, pre-pregnancy obesity, smoking and maternal medical conditions such hypertension, preeclampsia, diabetes, and abruptio placenta.

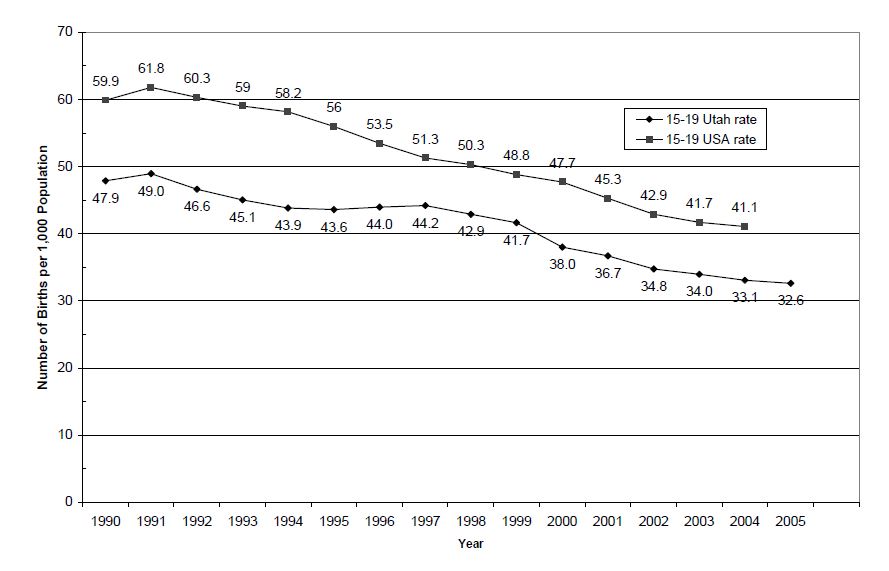
Analysis of Utah Fetal Death data 1992-2005 indicate that risk of fetal death was higher in younger (19) and older women (≥35), and risk increased with advancing maternal age.
Utah Data vs. U.S. (How are we doing?)
The fetal mortality rate in Utah is lower than the national rate, however, it is still above the Healthy People 2010 goal of 4.1 (Objective No. 16-1a). Although the rate decreased significantly over past decades, the problem of fetal mortality remains immense. During 2005 alone, 260 infants were stillborn in Utah.

Recommendation
It has been estimated that close to half of all fetal deaths have no identifiable causes. In order to decrease fetal mortality rate, it is essential to understand the etiology of fetal death. Such etiology will direct public health actions and will also influence future preconceptional counseling, pregnancy management, and neonatal care management. Preventive strategies should target research, improve fetal death surveillance and reporting, and educate practitioners in identifying women at risk. (3)
The National Institute of Child Health and Human Development recently awarded grants to five sites for population-based studies on fetal death. The Division of Maternal-Fetal Medicine at the University of Utah is one of the sites that will focus on studying stillbirth.
References
- Fretts, RC; Usher, RH. (1997). Causes of fetal death in women of advanced maternal age. Obstet Gynecol, Vol 89, p 40-45.
- Cande, V; Ananth, PhD, MPH; Shiliang, L, PhD, MB; Kinzler,WL, MD; Kramer, MS, MD. (2005. Stillbirths in the United States, 1981–2000: An age, period, and cohort analysis. American Journal of Public Health, Vol 95, No. 12, p 2213-2217
- Barfield, W; and Martin, J. (June 25, 2004). Racial /ethnic trends in fetal mortality–United States, 1990-2000. MMWR, Vol. 53 (24); p 529-532.